Chapter: Microbiology and Immunology: Virology, Virus: Papovaviruses
Pathogenesis and Immunity - Human Papillomaviruses
Pathogenesis and Immunity
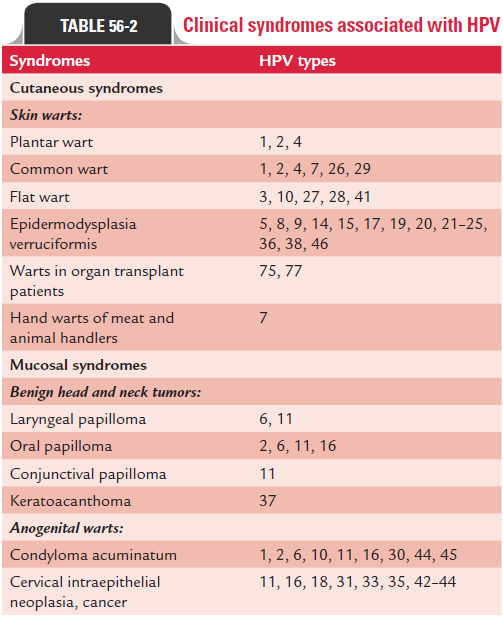
Human papilloma viruses show high degree of host specific-ity. They show a high predilection for the skin and also for mucous membrane. HPV infection is acquired by close con-tact, and the infection is initiated by infections of the skin or mucous membranes. Tissue tropism and manifestation of the disease depend on the HPV type that causes disease (Table 56-2).
Pathogenesis of human papilloma virus infections
After infection, the virus replicates in the squamous epithe-lium of the skin to cause warts and in the mucous membrane to induce epithelial proliferation, such as oral, genital, and conjunctival papillomas. The warts occur as a result of virus-caused cell growth and thickening of the basal and prickle lay-ers of the stratum spinosum as well as the stratum granulosum.
The presence of the koilocytes is the hallmark of the HPV infections of the skin. These koilocytes are the enlarged keratocytes with well-demarcated halos surrounding small nuclei. The HPV infection always causes a localized infection and the warts usually resolve spontaneously possibly as a result of immune response.
Human papilloma virus has also been associated with devel-opment of oral premalignant conditions as well as malignant conditions in humans. HPV-16 as well as HPV-18, HPV-33, and HPV-35 have been linked with (a) verruciform proliferation in the oral cavity, (b) oral premalignant lesions, and (c) oral squamous cell carcinoma.
◗ Host immunity
The exact mechanism responsible for resolution of papillomas is not known. Cell-mediated immunity, however, appears to play an important role in the resolution of the disease. The con-ditions that depress cell-mediated immunity, such as in patients with HIV and those receiving immunosuppressive therapy, give rise to exacerbation of HPV infection and leads to more severe manifestation of the disease.
Related Topics