Chapter: Paediatrics: Inherited metabolic disease
Paediatrics: Disorders of porphyrin metabolism
Disorders of porphyrin metabolism
The porphyrins are the main
precursors of haem, and essential constit-uents of haemoglobin, myoglobin, the
respiratory and P450 liver cyto-chromes, and of other enzymes (catalases and
peroxidases). Deficiency in porphyrin pathway leads to accumulation of
precursors, which are toxic to tissues in high concentration. The chemical
properties of these precur-sors determines the site of tissue accumulation, and
whether they induce photosensitivity.
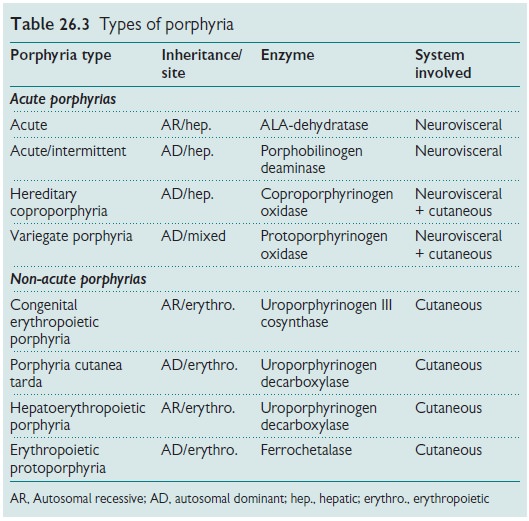
The porphyrias (Table 26.3) may be
inherited or acquired. They are broadly classified as hepatic porphyrias or
erythropoietic porphyrias, based on the site of the overproduction and main
accumulation of the porphyrins. They manifest with either skin problems or with
neurological complications (or occasionally both) and present either acutely or
non-acutely.
•
Hepatic porphyrias: are characterized by acute
neurological attacks manifesting as
seizures, neuropathy, behaviour problems/pyschosis, and hallucinations. Muscle
(back) pain, vomiting, and abdominal pain are also common. Acute episodes may
be triggered by exposure to certain drugs (e.g. alcohol, oral contraceptive
agents, and certain antibiotics) and by other chemicals and certain foods.
Fasting can also trigger attacks.
•
Erythropoietic porphyrias: present with skin problems,
including light-sensitive blistering rash and increased hair growth.
Spectroscopic and biochemical
analysis for abnormalities in porphyrin metabolite profile in urine and stools
is required for diagnosis. In nearly all cases of acute porphyria syndromes,
urinary porphobilinogen is markedly elevated (except in ALA dehydratase
deficiency).
Treatment
Acute porphyria
High carboydrate diet and
avoidance of precipitating factors. Haemearginate (early in acute episode).
Symptomatic treatment.
Erythropoietic porphyrias
The skin rash that occurs in erythropoietic porphyrias generally requires use of sunscreens and avoidance of bright sunlight. Chloroquine may be used to increase porphyrin secretion.
Related Topics