Chapter: Medical Physiology: Resistance of the Body to Infection: I. Leukocytes, Granulocytes, the Monocyte-Macrophage System, and Inflammation
Monocyte-Macrophage Cell System (Reticuloendothelial System)
Monocyte-Macrophage Cell System (Reticuloendothelial System)
In the preceding paragraphs, we described the macrophages mainly as mobile cells that are capable of wandering through the tissues. However, after entering the tissues and becoming macrophages, another large portion of monocytes becomes attached to the tissues and remains attached for months or even years until they are called on to perform specific local protective functions. They have the same capabilities as the mobile macrophages to phagocytize large quantities of bacteria, viruses, necrotic tissue, or other foreign particles in the tissue. And, when appropriately stimulated, they can break away from their attach-ments and once again become mobile macrophages that respond to chemotaxis and all the other stimuli related to the inflammatory process.Thus, the body has a widespread “monocyte-macrophage system” in vir-tually all tissue areas.
The total combination of monocytes, mobile macrophages, fixed tissue macrophages, and a few specialized endothelial cells in the bone marrow, spleen, and lymph nodes is called the reticuloendothe-lial system. However, all or almost all these cells orig-inate from monocytic stem cells; therefore, the reticuloendothelial system is almost synonymous with the monocyte-macrophage system. Because the term reticuloendothelial system is much better knownin medical literature than the term monocyte-macrophage system, it should be remembered as ageneralized phagocytic system located in all tissues, especially in those tissue areas where large quantities of particles, toxins, and other unwanted substances must be destroyed.
Tissue Macrophages in the Skin and Subcutaneous Tissues (His-tiocytes). Although the skin is mainly impregnable toinfectious agents, this is no longer true when the skin is broken. When infection begins in a subcutaneous tissue and local inflammation ensues, local tissue macrophages can divide in situ and form still more macrophages. Then they perform the usual functions of attacking and destroying the infectious agents, as described earlier.
Macrophages in the Lymph Nodes. Essentially no particu-late matter that enters the tissues, such as bacteria, can be absorbed directly through the capillary membranes into the blood. Instead, if the particles are not destroyed locally in the tissues, they enter the lymph and flow to the lymph nodes located intermittently along the course of the lymph flow. The foreign parti-cles are then trapped in these nodes in a meshwork of sinuses lined by tissue macrophages.
Figure 33–3 illustrates the general organization of the lymph node, showing lymph entering through the lymph node capsule by way of afferent lymphatics, then flowing through the nodal medullary sinuses, and finally passing out the hilus into efferent lymphatics that eventually empty into the venous blood.
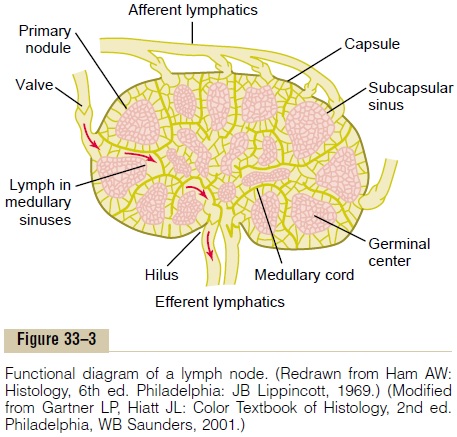
Large numbers of macrophages line the lymph sinuses, and if any particles enter the sinuses by way of the lymph, the macrophages phagocytize them and prevent general dissemination throughout the body.
Alveolar Macrophages in the Lungs. Another route bywhich invading organisms frequently enter the body is through the lungs. Large numbers of tissue macrophages are present as integral components of the alveolar walls. They can phagocytize particles that become entrapped in the alveoli. If the particles are digestible, the macrophages can also digest them and release the digestive products into the lymph. If the particle is not digestible, the macrophages often form a “giant cell” capsule around the particle until such time—if ever—that it can be slowly dissolved. Such capsules are frequently formed around tuberculosis bacilli, silica dust particles, and even carbon particles.
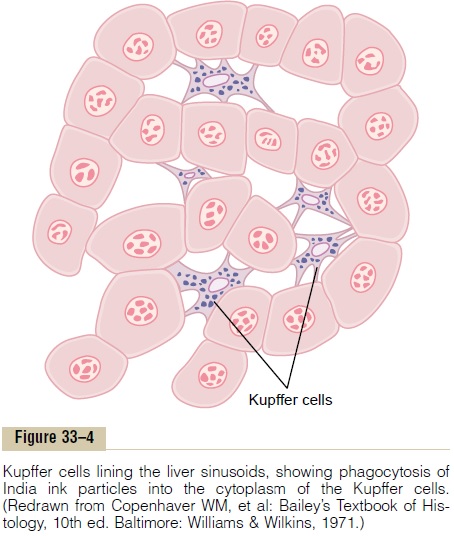
Macrophages (Kupffer Cells) in the Liver Sinusoids. Stillanother favorite route by which bacteria invade the body is through the gastrointestinal tract. Large numbers of bacteria from ingested food constantly pass through the gastrointestinal mucosa into the portal blood. Before this blood enters the general cir-culation, it passes through the sinusoids of the liver; these sinusoids are lined with tissue macrophages called Kupffer cells, shown in Figure 33–4. These cells form such an effective particulate filtration system that almost none of the bacteria from the gastrointestinal tract succeeds in passing from the portal blood into the general systemic circulation. Indeed, motion pictures of phagocytosis by Kupffer cells have demonstrated phagocytosis of a single bacterium in less than 1/100 of a second.
Macrophages of the Spleen and Bone Marrow. If an invad-ing organism succeeds in entering the general circula-tion, there are other lines of defense by the tissue macrophage system, especially by macrophages of the spleen and bone marrow. In both these tissues, macrophages have become entrapped by the reticular meshwork of the two organs, and when foreign parti-cles come in contact with these macrophages, they are phagocytized.
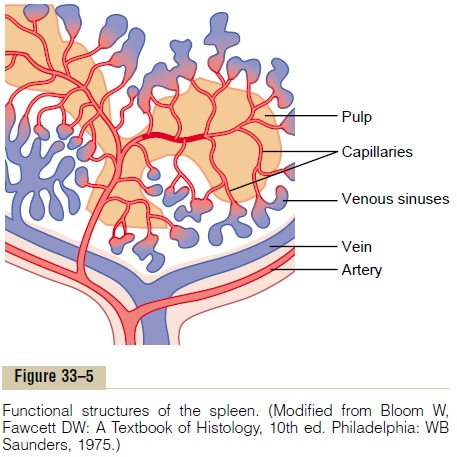
The spleen is similar to the lymph nodes, except that blood, instead of lymph, flows through the tissue spaces of the spleen. Figure 33–5 shows a small periph-eral segment of spleen tissue. Note that a small artery penetrates from the splenic capsule into thesplenicpulp and terminates in small capillaries. The capillar-ies are highly porous, allowing whole blood to pass out of the capillaries into cords of red pulp. The blood then gradually squeezes through the trabecular meshwork of these cords and eventually returns to the circulation through the endothelial walls of the venous sinuses. The trabeculae of the red pulp are lined with vast numbers of macrophages, and the venous sinuses are also lined with macrophages. This peculiar passage of blood through the cords of the red pulp provides an exceptional means of phagocytizing unwanted debris in the blood, including especially old and abnormal red blood cells.
Related Topics