Chapter: Medical Microbiology: An Introduction to Infectious Diseases: Central Nervous System Infections
General Diagnostic Approaches - Central Nervous System Infections
GENERAL DIAGNOSTIC APPROACHES
Except in unusual circumstances, in which severe increases in intracranial pressure make the procedure dangerous, a lumbar puncture is the first step in the workup of a patient with suspected CNS infection. The CSF pressure is determined at the time of the proce-dure, and CSF is removed for analysis of cells, protein, and glucose. Ideally, the glucose content of the peripheral blood is determined simultaneously for comparison with that in the CSF. Table 67–4 presents guidelines for interpretation of results of CSF analysis; these guidelines represent generalizations, however, and must not be considered as ab-solute findings in all cases. For example, although a patient with bacterial, mycobacterial, or fungal meningitis usually has a glucose level in the CSF of less than 40 mg/dL, or less than half the blood glucose level (hypoglycorrhachia), this finding may not be present in the early stages of infection. Viral infections of the CNS can occasionally produce low glucose values in the CSF; in addition, the early stages of viral infection may be associ-ated with a preponderance of polymorphonuclear leukocytes. It is clearly important to recognize that viral CNS infections can exist with a negligible CSF cell count. This some-times also occurs in the early stages of bacterial meningitis.
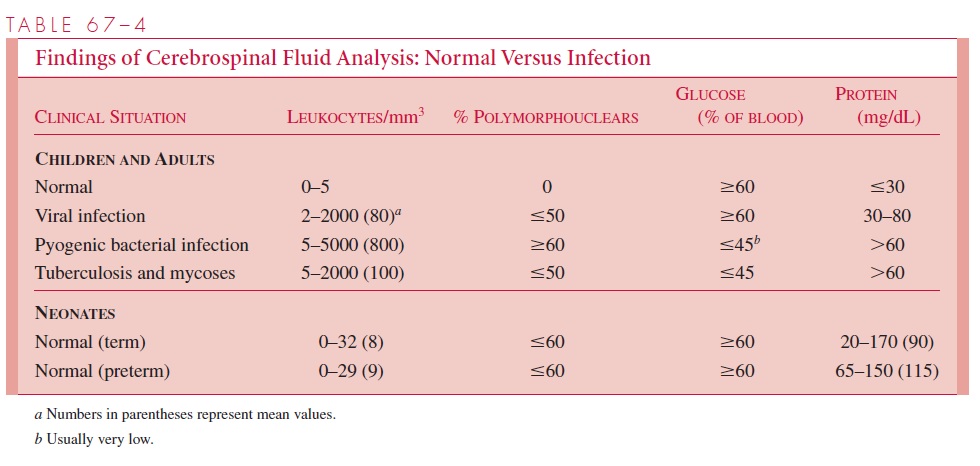
Realizing the limitations, it is possible to make some general interpretations that are helpful in the diagnosis. Viral CNS infections are usually associated with a preponder-ance of lymphocytes, a normal glucose value, and a normal or moderately elevated pro-tein level in the CSF. In contrast, acute bacterial meningitis usually causes a CSF pleocy-tosis consisting primarily of polymorphonuclear cells, a low glucose value, and a high protein level. Mycobacterial and fungal infections are more commonly associated with lymphocytosis (and sometimes moderate eosinophilia) in the CSF; like the acute bacterial infections, however, they tend to lower glucose and increase protein levels markedly.
Normal values for CSF are also shown in Table 67–4. Polymorphonuclear cells are not usually seen in normal CSF, but as many as five lymphocytes/mm3 may be found in healthy individuals. Neonatal CSF is considerably more difficult to interpret, because cell counts are often elevated in the absence of infection; glucose values, however, should be within the normal range.
The other major procedures that must be performed on all CSF samples in which any infection is suspected include bacterial cultures and Gram staining. If the CSF is grossly purulent and the patient untreated, a Gram stain of the uncentrifuged CSF or of its cen-trifuged sediment frequently shows the infecting organism and indicates the specific diag-nosis. According to the clinical indications and results of CSF cytology and chemistry, other microbiologic tests may be used, including viral cultures, special stains and cultures for fungi and mycobacteria, immunologic methods to detect fungal or bacterial antigens (eg, latex agglutination for Cryptococcus), and polymerase chain reactions to detect viral or bacterial nucleic acids.
Tests on specimens other than CSF are selected on the basis of the clinical diagnostic possibilities. If acute bacterial meningitis is suspected, blood cultures should also be used to ensure the diagnosis. Viral cultures of the pharynx, stool, or rectal swabs may provide indirect evidence of CNS infection. In encephalitis, a biopsy specimen of the brain is sometimes obtained for culture, histology, and to demonstrate viral antigen or nucleic acid. Other studies may include acute and convalescent sera for viral serology and sero-logic tests to detect antibodies to certain fungi, such as C. immitis.
Intracranial abscesses can often be detected with radiologic techniques, such as com-puterized tomography or magnetic resonance imaging. A definitive etiologic diagnosis is established by careful aerobic and anaerobic culture of the contents of the abscess.
Related Topics