Chapter: Ophthalmology: Sclera
Episcleritis
Episcleritis
Definition
Circumscribed, usually segmental, and
generally nodular inflammation of the
episclera (connective tissue between sclera and conjunctiva).
Epidemiology:
Episcleritis is the most common form of scleral inflammation.
Etiology:
Episcleritis is rarely attributable to one of
the systemic underlyingdisorders listed in Table 6.1, and is only occasionally due to bacterial or viral inflammation.
Often episcleritis will have no readily discernible cause.

Symptoms:
Episcleritis can be unilateral or bilateral.
It is usually associatedwith segmental reddening and slight tenderness to
palpation.
Findings:
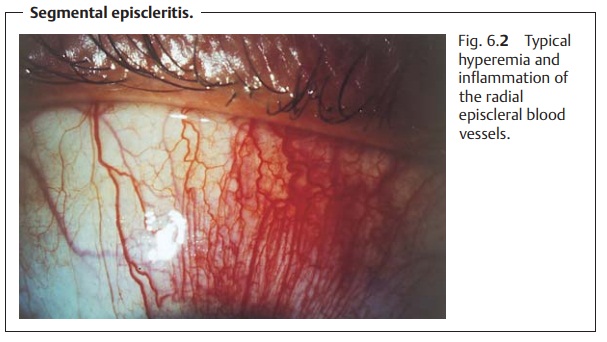
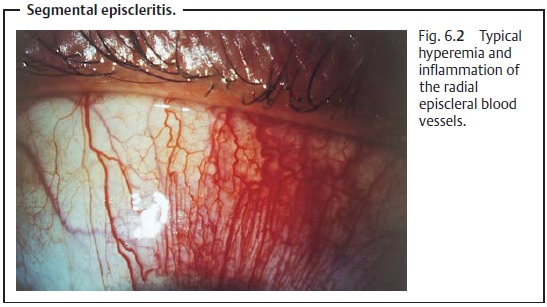
The episcleral vessels lie within the fascial
sheath of the eyeball(Tenon’s capsule) and are arranged radially. In
episcleritis, these vessels and the conjunctival vessels above them become
hyperemic (Fig. 6.2). Tenon’s
capsule and the episclera are infiltrated with inflammatory cells, but the
sclera itself is not swollen. The presence of small mobile nodules is typical of nodular episcleritis.
Differential diagnosis:
The disorder should be distinguished from
conjunctivitis (see next paragraph) and scleritis (6.6.2).
The conjunctival blood vessels are the most
superficial; the episcleral vessels lie within Tenon’s capsule and are arranged
radially. When vaso-constrictive eyedrops are applied, the conjunctival
injection will disap-pear but not the episcleral injection. This makes it possible
to distin-guish conjunctivitis from episcleritis.
Treatment and prognosis:
Episcleritis usually resolves
spontaneouslywithin one to two weeks, although the nodular form can persist for
extended periods of time. Severe symptoms are treated with topical steroids
(eyedrops) or with a nonsteroidal anti-inflammatory agent.
Related Topics