Chapter: Pathology: Endocrine Pathology
Diabetes Mellitus
DIABETES MELLITUS
Diabetes mellitus (DM) is a
chronic systemic disease characterized by insulin defi-ciency or peripheral
resistance, resulting in hyperglycemia and nonenzymatic glycosylation of
proteins. Diagnosis is established by demonstrating either of the following:
•
Fasting glucose >126 mg/dL on at least 2 separate occasions
•
Positive glucose tolerance test
A glycated hemoglobin (HbA1c)
assay is used for certain patient populations. The diagnostic cutoff is 6.5%.
Type 1 diabetes (T1D) represents
10% of cases of diabetes.
•
Affects children and adolescents, usually age <20
•
Risk factors include Northern European ancestry and specific HLA types
(DR3, DR4, and DQ)
•
Pathogenesis is a lack of insulin due to autoimmune destruction of β
cells (type IV hypersensitivity reaction)
•
Patients are absolutely dependent on insulin to prevent ketoacidosis and
coma
•
Thought to be caused by autoimmune reaction triggered by an infection
(Cox-sackie B virus) in a genetically susceptible individual
T1D can present with polydipsia,
polyuria, and polyphagia; dehydration and elec-trolyte imbalance; metabolic
ketoacidosis; and coma and potentially death. Micro-scopically, lymphocytic
inflammation involves the islets of Langerhans (insulitis), leading to loss of
β cells and fibrosis of the islets. Treatment is insulin.
Type 2 diabetes (T2D) represents
90% of cases.
•
Affects obese individuals, both children and adults
•
Approximately 10 million people in the United States are affected (half
are undiagnosed), and incidence increases with age
•
Risk factors include obesity, increasing age, and genetic predisposition
•
Pathogenesis involves relatively reduced insulin secretion; peripheral
insulin resistance is the term used for reduced tissue sensitivity to insulin
due to decreased numbers of insulin receptors on the cell membranes.
T2D is often asymptomatic, but
it can present with either polydipsia, polyuria, and polyphagia, or with
hyperosmolar nonketotic diabetic coma. Microscopically, the changes are
nonspecific, and can include focal atrophy and amyloid deposition in islets
(hyalinization). Treatment is diet/weight loss, oral antidiabetic drugs, and
insulin as needed (more common in long-standing cases).
Vascular pathology. Diabetes is a major risk factor for atherosclerosis and its
com-plications, including myocardial infarction (most common cause of death),
stroke (CVA), and peripheral vascular disease. The vascular disease can lead to
atrophy of skin and loss of hair of the lower extremities, claudication,
nonhealing ulcers, and gangrene of lower extremities.
Diabetic nephropathy includes glomerular lesions, arteriolosclerosis, and pyelone-phritis.
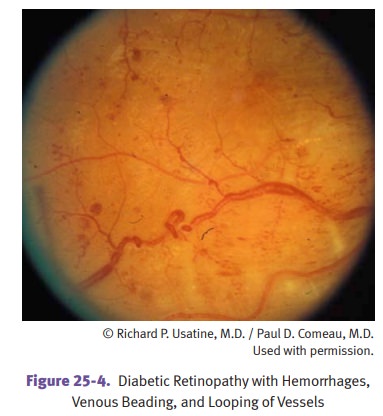
Diabetic retinopathy. Nonproliferative retinopathy is characterized
by microan-eurysms, retinal hemorrhages, and retinal exudates. Proliferative
retinopathy is characterized by neovascularization and fibrosis. Diabetics also
have an increased incidence of cataracts and glaucoma.
Diabetic neuropathy can cause peripheral neuropathy, neurogenic bladder, and sexual
impotence.
Related Topics