Chapter: Medical Microbiology: An Introduction to Infectious Diseases: Clostridium, Peptostreptococcus, Bacteroides, and Other Anaerobes
Clostridium Difficile Diarrhea
C .difficile DIARRHEA
C. dif cile is the most common cause of diarrhea that develops in association with the use of antimicrobial agents. The diarrhea ranges from a few days of intestinal fluid loss to life-threatening pseudomembranous colitis (PMC). This condition is associated with intense inflammation and the formation of a pseudomembrane composed of inflammatory debris on the mucosal surface.
EPIDEMIOLOGY
C. dif cile is present in 2 to 5% of the general population, sometimes at higher rates among hospitalized persons and infants. More than two decades of the antibiotic era had elapsed before the medical importance of C. dif cile was recognized through its association with antibiotic-associated diarrhea (AAD). Although infection is endogenous in most cases, hos-pital outbreaks have clearly established that the environment can be the source as well.C. dif cile is by no means the only cause of ADD, but it is the most common identifi- able cause. In simple diarrhea following antimicrobial administration, this organism is responsible for approximately 30% of cases. As the disease progresses to colitis, the asso- ciation is stronger, rising to 90% if PMC is present. Person-to-person transfer is very rare except in the instance of hospital-acquired C. dif cile infections, where environmental or hand contamination leads to infection of another patient.
PATHOGENESIS
When C. dif cile becomes established in the colon of individuals with normal gut flora, few if any direct consequences result, probably because its numbers are dwarfed by the other flora. Alteration of the colonic flora with antimicrobics (particularly ampicillin, cephalosporins, and clindamycin) favors C. dif cile in two ways.
First, strains resistant to the antimicrobic can grow in its presence and assume a larger if not dominant position in the ora. Second, in an antimicrobial milieu, the readiness with which C. dif cile forms spores may favor its survival over non – spore-forming bacteria. In either case, the minor niche of the species is improved to the point at which the effect of its toxins on the colonic mucosa becomes signi cant.
Although the vast majority of strains produce both toxins, the enterotoxic properties of the A toxin seem to dominate in watery diarrhea cases. In PMC, the colonic mucosa is studded with in ammatory plaques, which may coalesce into an overlying “pseudomem-brane” composed of brin, leukocytes, and necrotic colonic cells (Fig. 19 – 4). This picture ts better with the action of the c ytotoxic B toxin. It is intriguing that colonized newborn children, who lack the complex ora of adults, rarely suffer any clinical consequences even though toxin production can be demonstrated. The extent to which these differences are due to variability in toxin expression or intestinal receptors is unknown.
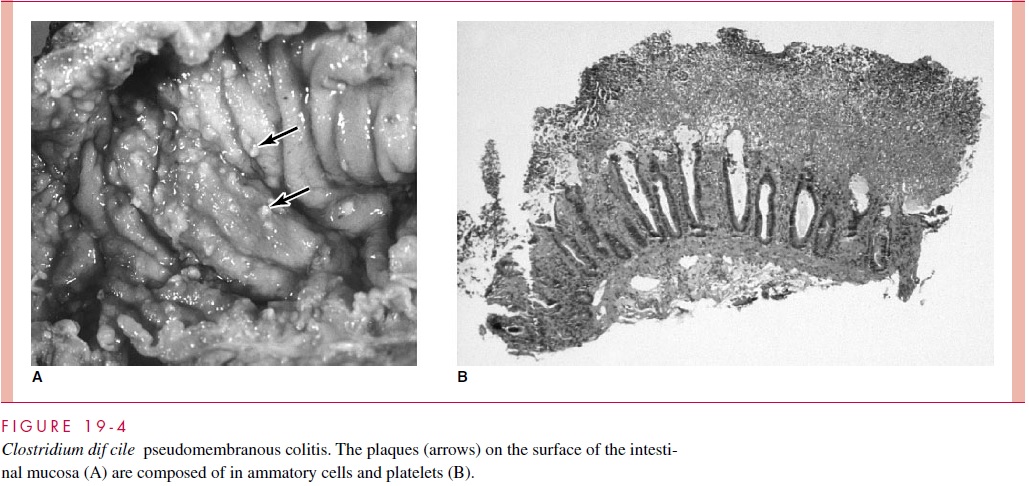
IMMUNITY
Antibody against the A toxin is associated with resolution of disease in experimental ani-mals. This feature and the inverse relationship between severity of disease and anti-A antibody both support the importance of humoral immunity in C. dif cile diarrhea. Anti-bodies directed against the B toxin also appear to offer protection, but the relationship is less clear than with toxin A.
Related Topics