Chapter: Nutrition and Diet Therapy: Diet and Diabetes Mellitus
Classification of Diabetes Mellitus
CLASSIFICATION
The types of diabetes
are prediabetes, type 1, type 2, and gestational. Prediabetes means that the
cells in the body are not using insulin properly. The diagnosis is made by a
fasting blood glucose, which is more than 110 but less than 126 mg/dl. One’s
lifestyle will determine when prediabetes will advance to type 2.
Type 1 diabetes develops when the
body’s immune system destroysthe pancreatic beta cells. These are the only
cells in the body that make the hormone insulin that regulates blood glucose.
Type 1 diabetes is usually diag-nosed in children and young adults. It can
account for 5% to 10% of all cases of newly diagnosed diabetes. Some risk
factors include genetics, autoimmune status, and environmental factors.
Type 2 diabeteswas previously called
adult-onset diabetes because itusually occurred in adults over the age of 40.
Type 2 is associated with obesity, and obesity has become an epidemic, which
has drastically increased the inci-dence of type 2 diabetes among adolescents
and young adults. A family history of diabetes, prior history of gestational
diabetes, impaired glucose tolerance, older age, physical inactivity, and race
and ethnicity can predispose one to type 2 diabetes. African Americans,
Hispanic and Latino Americans, Native Americans, some Asian Americans, and
Native Hawaiians and other Pacific Islanders are at particularly high risk for
type 2 diabetes. It is not uncommon for the client to have no symptoms of
diabetes and to be totally ignorant of hisor her condition until it is
discovered accidentally during a routine urine or blood test or after a heart
attack or stroke. In type 2 diabetes, hypertension may be present as part of
the metabolic syndrome (i.e., obesity, hypergly-cemia, and dyslipidemia) that is accompanied
by high rates of cardiovascular disease. The American Diabetes Association
recommends that blood pressure be controlled at >130/80 mm Hg for diabetics.
Type 2 diabetes can
usually be controlled by diet and exercise, or by diet, exercise, and an oral diabetes medication.
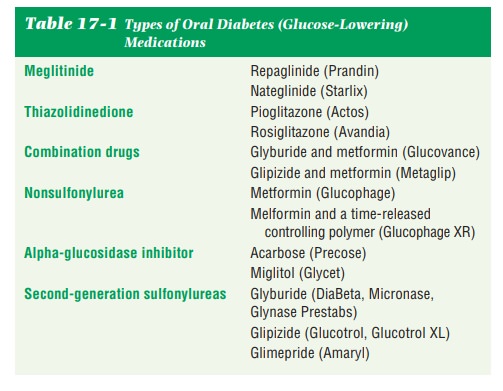
Table 17-1 shows six types of oral
glucose-lowering medications in order from newest and most frequently used to
oldest and least frequently used. The goals of medical nutri-tion therapy for
clients with type 2 diabetes include maintaining healthy glucose, blood
pressure, and lipid levels. Also, because approximately 80% of type 2 clients
are overweight, these clients may be placed on weight reduc-tion diets after
their blood glucose levels are within acceptable range. Thus, monitoring their
weight loss also becomes part of their therapy. Exenatide (Byetta) injection is
the first in a new class of drugs for the treatment of type 2 diabetes. The
drugs are called incretin mimetics. When food is eaten, incretin hormones are
released from cells located in the small intestine. In the pancreas, incretins
will act on the beta cells to increase glucose-dependent insulin secretions to
ensure an appropriate insulin response after a meal. This medication is used in
conjunction with the nonsulfonylurea metformin to help clients lower their
HgbA1c to less than 7%. HgbA1c is a blood test to determine
how well blood glucose has been controlled for the last 3 months. The American
Diabetes Association prefers the outcome be less than 6%.
Gestational diabetes
can occur between the sixteenth and twenty-eighth week of pregnancy. If it is
not responsive to diet and exercise, insulin injection therapy will be used
(Figure 17-1). It is recommended that a dietitian or a diabetic educator be
consulted to plan an adequate diet that will control blood sugar for mother and
baby.
Concentrated sugars
should be avoided. Weight gain should continue, but not in excessive amounts.
Usually, gestational diabetes disappears after the infant is born. However,
diabetes can develop 5 to 10 years after the pregnancy.
Secondary diabetes
occurs infrequently and is caused by certain drugs or by a disease of the
pancreas.
Related Topics