Chapter: Clinical Cases in Anesthesia : Respiratory Failure
Briefly describe the most common ventilatory modes
Briefly
describe the most common ventilatory modes.
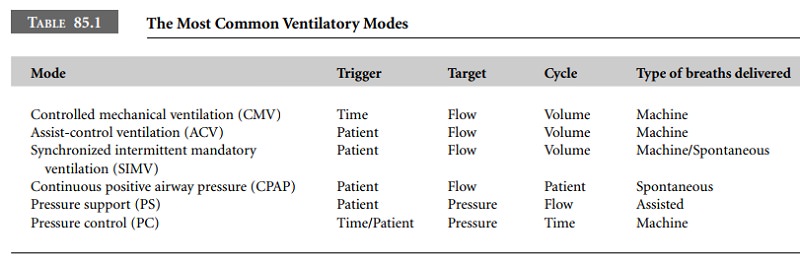
The most commonly used ventilatory modes are
detailed in Table 85.1. “Trigger” refers to the event that ini-tiates a breath.
The set trigger can be time, in which case the set rate determines how often a
breath will be delivered, or patient, in which case the ventilator will detect
an inspi-ratory effort by the patient. The inspiratory effort can be detected
either by the generation of negative pressure or inspiratory flow. “Target”
refers to the set point for the ven-tilator during the breath. The target can
be flow, in which case a set number of liters per minute will be delivered, or
pressure, in which case a set pressure is attained. “Cycle” designates the
event that terminates the breath. It can be volume, i.e., the set tidal volume
has been delivered, patient, for spontaneous breaths, flow, in which case the
breath is terminated when the inspiratory flow reaches 25% of the peak flow, or
time.
CMV is also called volume-controlled (VC)
ventilation. The respiratory rate and tidal volume are set on the venti-lator,
and the patient cannot take any spontaneous breaths.
It is only appropriate for a patient under deep
sedation, neuromuscular blockade, or general anesthesia.
Assist-control ventilation (ACV) allows a
patient to receive a preset number of machine breaths per minute. The
ventilator will detect additional inspiratory efforts by the patient and
deliver a machine breath with the set tidal volume.
Intermittent mandatory ventilation (IMV) is
remark-able in that it combines machine breaths at a set rate (breaths will be
synchronized with inspiratory efforts in synchronized intermittent mandatory
ventilation, SIMV) and spontaneous breaths, either without assistance, or,
almost exclusively nowadays, in combination with pressure support. It is used
to permit a patient to take additional breaths, or as a weaning mode by
progressively decreasing the rate of machine breaths.
Continuous positive airway pressure (CPAP) was
ini-tially devised as a mode to deliver PEEP to a spontaneously breathing
patient. Quite often, however, it is informally used to designate spontaneous
breathing on a ventilator, regard-less of whether the pressure is positive at
end-expiration.
Pressure support (PS) is used to assist
spontaneous breaths. The ventilator detects an inspiratory effort and maintains
a preset pressure until the inspiratory flow drops to 25% of the peak flow. A
pressure support of 5–10 cm H2O should be equivalent to breathing
spontaneously without an endotracheal tube. It compensates for the resistance
of the endotracheal tube, the ventilator tubing, and valves. A higher value
provides additional support. This mode is mainly used for weaning from the
ventilator. The controversy as to the best weaning mode—SIMV with PS versus PS
alone—is far from resolved.
Pressure control (PC) was devised to limit
hyperinsuf-flation, especially in patients with ARDS. It can be delivered as
either CMV or ACV. Tidal volume is not set. Instead, a target pressure and an
inspiratory time are programmed. Thus, the tidal volume received by the patient
will depend on lung and chest wall compliance. This has not been shown to
improve outcome.
Related Topics