Chapter: Surgical Pathology Dissection : The Central Nervous System
Brain and Spinal Cord : Surgical Pathology Dissection
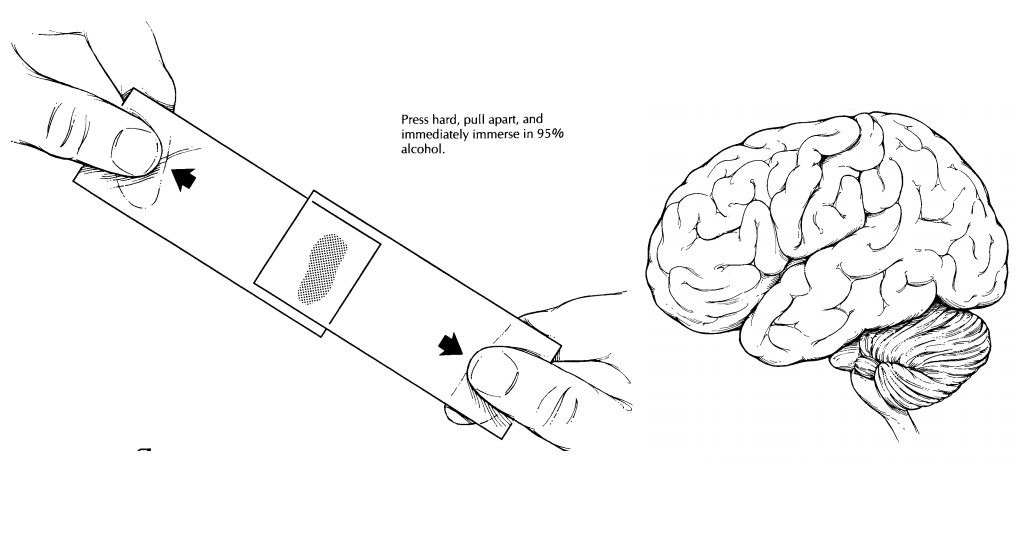
Brain and Spinal Cord
General Comments
In some
respects, pathologic evaluation of speci-mens from the central nervous system
(CNS) is less complicated than evaluation of other or-gans, because requests
for margins and the need for extensive specimen dissections are unusual. On the
other hand, CNS specimens are usually small, and care must be taken to preserve
the tis-sue. Do not use all of the tissue by freezing the entire specimen. This
is especially true for speci-mens of the spinal cord. These can be minute, yet
major therapeutic decisions often depend on the results of the pathology
studies. In all cases, it is essential to keep the clinical and radiologic
findings in mind when processing specimens from the CNS.
Ultrasonic
aspirations are widely used for tumor resections. As a consequence, much of the
specimen may be lost unless it is recovered from the instrument’s bag
receptacle. The fragments may be difficult to interpret histologically but can
be invaluable. They are entirely suitable for molecular or cytogenetic studies.
Cytologic Preparations
Cytologic
preparations are essential in the frozen section and permanent section
evaluation of all surgically excised brain lesions. These should be prepared in
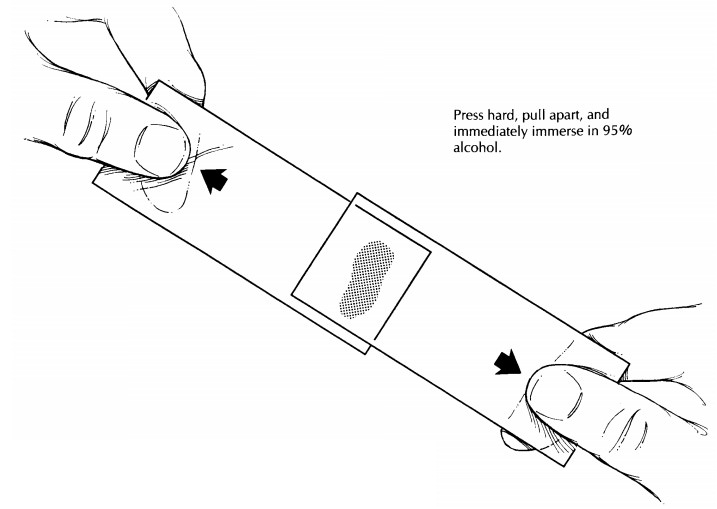
every case for which a frozen section is requested. As illustrated, the
preferred proce-dure is as follows: A minute portion of the fresh specimen is
placed on a glass slide and, with con-siderable pressure, smeared between an
oppos-ing slide. The slides are separated and immersedimmediately in 95% alcohol. Following fixation for45 to 60 seconds,
the preparation is stained and coverslipped. I prefer routine staining with
hema-toxylin and eosin.
Needle Biopsy Specimens
Needle
biopsy specimens need to be interpreted and handled with special care. The
evaluation should begin with cognizance of the clinical and radiographic
findings. The chance of making an error is vastly increased when these
specimens are studied in a vacuum devoid of clinical or radiographic information.
Begin
your examination with the cytologic preparation as described above. One of the
re-maining fragments of tissue can then be used for a frozen section if
desired. If an abnormality is established by the smear, a frozen section may
not be necessary. Unless you are assured of addi-tional tissue, it is generally
wise to freeze only one or two cores at the time of initial examination,
holding others in reserve. Throughout the pro-cess, review these slides in
reference to the ra-diographic images to ensure that abnormal tissue is
obtained and that the findings are consistent with the images. Close contact
with the surgeon is extremely important. As is true for biopsies from other
body sites, small specimens can be colored with eosin to facilitate identification
at the time of embedding and sectioning.
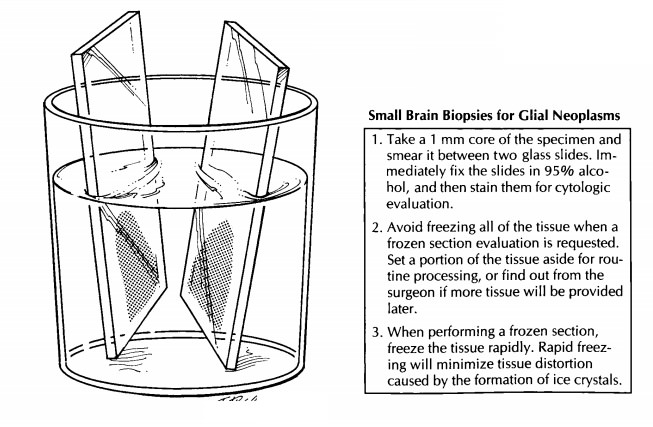
Frozen Sections/Permanent Sections
Freezing
must be accomplished as rapidly as pos-sible to minimize the formation of ice
crystals.
Ice
crystals are generally avoidable in certain neo-plasms, such as meningiomas,
but frequently not in infiltrating gliomas from edema-rich white matter. The
recommended procedure is to estab-lish a base of semifrozen mounting medium on
a cold chuck. The medium should not be com-pletely frozen, because solidly
frozen medium will slowly freeze the tissue and encourage the formation of ice
crystals by gradually drawing heat from the small specimen. Therefore, place
the specimen on the partially frozen base, and immediately immerse it in liquid
nitrogen. After freezing, the specimen can then be covered with additional
mounting medium and refrozen. Cut and stain sections by standard methods.
In the
case of gliomas, especially the well-differentiated variety (e.g., astrocytoma
and oli-godendroglioma), it is extremely important that blocks be available
from tissue that is not subject to
prior frozen section. Prior freezing produces nuclear angulation and
hyperchromatism, which can make it difficult to distinguish between glio-mas
and to distinguish reactive or normal brain from an infiltrating glioma. Unless
you are as-sured of more tissue by the surgeon, use only a portion of the
specimen for a frozen section.
Electron Microscopy
To a
large extent, immunohistochemistry has re-placed electron microscopy as a
diagnostic tool; however, in certain instances the latter technique is
invaluable. Accordingly, it is appropriate to hold some tissue in reserve in
glutaraldehyde (embedding later if necessary) for neoplasms for which
classification may be difficult after review of the frozen section. Tissue may
also be embed-ded from encephalitic lesions if viruses are sus-pected, because
no immunohistochemical agents are commercially available for many classes of
potential viral pathogens.
Processing of Tissues From Specific Entities
Meningiomas
are frequently submitted with a dural attachment and arrive as either a
complete en bloc excision or, more often, as a series of small fragments.
Prognostically significant informationrelates to histologic features of the
lesion as well as the interface of the tumor with surrounding tissues, that is,
the brain and the skull. The surface of the mass adjacent to the brain should
be sec-tioned, if identified, particularly if portions of the brain adhere to
the surface. At least one section through the base of the tumor on the dura
should also be taken. Decalcified sections of bone are appropriate to evaluate
skull invasion.![]()
Gliomas
are an exceedingly heterogeneous group in terms of their macroscopic and
micro-scopic characteristics. Generally, margins are not an issue and do not,
unless specifically stated by the surgeon, affect the treatment of the patient.
Fragments of ependymomas, oligodendroglio-mas, and astrocytomas, in which
little normal brain is recognized, do not need to be sampled in regard to the
extent of the disease, although it is prudent to attempt such a localization.
In larger en bloc specimens of gliomas, however, a series of marked and
recorded sections passing from the tumor into the macroscopically normal brain
is appropriate. In the case of malignant gliomas with central necrosis, the
most diagnostic tissue is usually found in the cellular rim immediately
surrounding the necrotic area. Sections from this area are therefore
appropriate. In the case of well-differentiated gliomas (e.g., astrocytoma and
oligodendroglioma), the tissue may not appear markedly abnormal, and multiple
sections are necessary, particularly from areas in which the white matter is
discolored.
Malignant
gliomas after radiotherapy may have extensive therapy-related changes, such as
coagulation necrosis. In this setting, multiple tissue sections should be
submitted so as not to miss potential foci of active recurrent tumor.
Oligodendrogliomas
are increasingly diag-nosed by molecular techniques. The molecular laboratory
can be consulted in regard to specific tissue preparation (e.g., fresh frozen,
etc...).
Lymphomas
are generally recognized during the frozen section process and, in the sporadic
form in the nonimmunocompromised patient, they are often suspected on the basis
of the neuroimaging features. In this setting, tissue can be reserved frozen
for special marker studies, although most of the relevant markers for the
simple purpose of establishing a clinical diagnosis can be performed on
paraffin-embedded sections. A clinical history of prebi-opsy steroid treatment
is significant, as CNS lymphomas in this setting may be little more thana mass
of macrophages and few if any residual neoplastic cells.
Pituitary
adenomas are often approached via the transsphenoidal route, and the specimens
are often small. Care must be taken not to freeze all of the specimens, as the
resultant artifact complicates interpretation of permanent sections. Close
com-munication with the surgeon is essential.
Creutzfeldt-Jakob
disease is a rare disorder that is occasionally diagnosed in a cortical biopsy
specimen. Although there appears to be only a very small likelihood that
pathology person-nel will contract Creutzfeldt-Jakob disease from these
specimens, caution is appropriate consider-ing the devastating consequences of
this disease. Details of this issue are discussed by Brown.20Basically,
the tissues are fixed in a standard for-malin solution for at least 48 hours.
The tissues are then placed in a cassette and decontaminated by immersion with
periodic agitation in a 95% formic acid solution. The tissue will turn clear.
After this, the tissue is placed in formalin again for 1 to 2 days. The tissues
can then be treatedas any other routine specimen, although some laboratories
prefer to hand process them sepa-rately. Generally, frozen sections are not
recom-mended on tissues from demented patients.
Specimens
taken to control seizures are usually from the temporal lobe. Often they
consist of “lateral” and “medial” temporal lobe specimens. The latter contains the
hippocampus, which must be examined carefully for the presence or absence of
“mesial” or “hippocampal” sclerosis (i.e., neu-ronal loss and gliosis).
Important Issues to Address in Your Surgical Pathology Report on Brain and Spinal Cord Biopsies
• What procedure
was performed?
• What are
the type and grade of the neoplasm? (For glial neoplasms, be sure to document
the grading system employed.)
• What is
the size of the neoplasm?
Related Topics