Chapter: Microbiology and Immunology: Immunohematology
ABO Blood Group System and Antigens
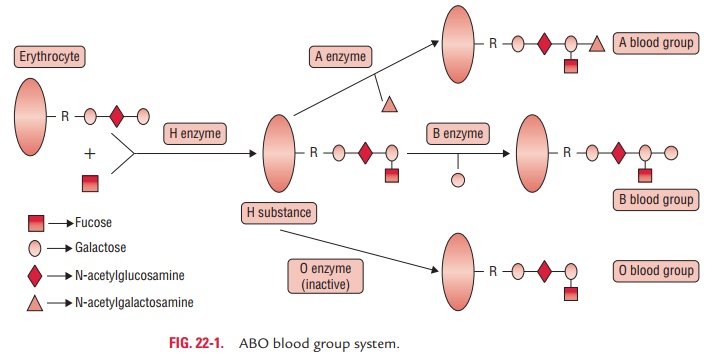
ABO Blood Group System
ABO blood group system was the first human red-cell antigen system to be characterized. The ABO blood group substances are glycopeptides with oligosaccharide side chains (Fig. 22-1). The ABO blood group specificity is determined by the presence of terminal sugar in an oligosaccharide structure. The terminal sugars of the oligosaccharides are specific for blood groups A and B. They are also immunogenic. The red cells express either A, B, both A and B, or neither, and antibodies are found in serum to antigens not expressed by the red cells.
ABO Blood Group Antigens
The blood group of an individual is determined by presence or absence of two antigens, A and B, on the surface of the red cell membrane. Red cells of blood group A carry antigen A, cells of blood group B carry antigen B, and cells of blood group AB have both A and B antigens. On the other hand, blood group O cells have neither A nor B antigens.
The blood groups are also differentiated by the presence or absence of two distinct isoantibodies in the serum. Serum of blood group A individuals have anti-B antibodies, blood group B have anti-A antibodies, and blood group O have both anti-A and anti-B antibodies. The blood group AB does not contain any anti-A and anti-B antibodies in the serum.
Soluble ABO blood group substances may be found in mucous secretions of humans, such as saliva, gastric juice, ovarian cyst fluid, etc. Such persons are termed secretors, while those without the blood group substances in their secretions are nonsecretors.
The ABO group of a given individual is determined by test-ing both cells and serum. In this method, the subject’s red cells are mixed with serum containing known antibody and the sub-ject’s serum is tested against cells possessing known antigen. For example, the cells of a group A individual are agglutinated by anti-A serum but not by anti-B serum, and his or her serum agglutinates type B cells but not type A cells. The typing of cells as group O is done by exclusion (a cell not reacting with anti-A or anti-B is considered to be of blood group O). It is noteworthy that these antibodies to the isoantigens are found in all individuals including those that have had no transfusions.
It is believed that the anti-A and anti-B isoagglutinins are synthesized as a consequence of cross-immunization with bac-teria of the family Enterobacteriaceae that colonize the infants’ gut. These bacteria have outer membrane oligosaccharides strikingly similar to those that define the A and B antigens in the human body. For example, a newborn with group A will not have anti-B in his or her serum, since there has been no oppor-tunity to undergo cross-immunization. When the intestine is eventually colonized by the normal microbial flora, the infant will start to develop anti-B, but will not produce anti-A because of tolerance to his or her own blood group antigens. The inheri-tance of the ABO groups follows simple Mendelian rules, with three common allelic genes: A, B, and O (A can be subdivided into A1 and A2), and any individual will carry two alleles, one inherited from the mother and one from the father.
◗ H antigen
Red cells of all ABO groups possess a common antigen, the H anti-gen, or H substance. H antigen is a glycoprotein and structurally is an L-fucose. It is a precursor for the production of A and B antigens. A and B antigens are formed by addition of N-acetylgalactosamine and galactose, respectively, to L-fucose of H antigen.
The H antigen, due to its universal distribution, is not that important in blood grouping or transfusion. However, in rare instances, such as in “Bombay,” or OH blood, both A and B anti-gens as well as H antigens are absent in the blood. Individuals with “Bombay” blood group have anti-A, anti-B, and anti-H antibodies, hence are not compatible with most of the red cells.
Related Topics