Chapter: Microbiology and Immunology: Applied Microbiology: Normal Microbial Flora
Normal Flora at Various Sites of the Body
Normal Flora at Various Sites of the Body
Respiratory Tract
Respiratory tract is subdivided into (a) the upper airways, which include the anterior and posterior nares and the nasopharynx; (b) the middle airways comprising the oropharynx and tonsils; and (c) the lower airways with larynx, trachea, bronchi, and lungs. The structural and physiological differences at each site provide an environment compatible for some organisms and hostile for others.
◗ Nares and nasopharynx
Nares are inhabited by a small number of organisms, which include Staphylococcus, Corynebacterium, Peptostreptococcus, and Fusobacteriumspecies. The microbial population in the nasopharynx is more complex with the predominance of streptococci and Neisseria species. Streptococcus salivarius, Streptococcus parasanguis, and Streptococcus pneumoniae can bereadily recovered from the nasopharynx. Twelve species of Neisseriahave been recovered from nasopharyngeal carriers.Colonization with Neisseria meningitidis varies from 10% to 95% with the highest incidence in young adults. Other Neisseria species that colonize the nasopharynx are Neisseria subflava, Neisseria sicca, Neisseria mucosa, and Neisseria lactamica. Gram-negative coccobacilli that colonize the nasopharynx include Moraxella catarrhalis and Kingella species. Noncapsulatedstrains of Haemophilus influenzae are also commonly found in the nasopharynx.
◗ Oropharynx and tonsils
The oropharynx is a complex mixture of ecosystems. Gram-positive and Gram-negative cocci predominate in the oropharynx. Overall, anaerobes outnumber aerobes with a ratio of 100:1. The most common anaerobic bacteria present in the oropharynx are Peptostreptococcus, Veillonella,Actinomyces, and Fusobacterium, whereas the most common aerobic bacteria are Streptococcus and Neisseria. Nearly 20% of individuals are colonized with Staphylococcus aureus. Streptococcus species that colonize the oropharynx are S. salivarius (saliva), Streptococcussanguis and S. mutans (tooth surface), Streptococcus vestibularis and S. sanguis (oral mucosa), S. pneumoniae, and beta-hemolytic streptococci. Other Gram-positive cocci that are present in the oropharynx include Stomatococcus mucilaginosus, Gemella species, etc.
Gram-negative cocci and coccobacilli also colonize the oropharynx. Veillonella, anaerobic Gram-negative cocci, are the most numerous Gram-negative cocci found in the oropharynx. Other Gram-negative cocci include Neisseria, Moraxella, Kingella, Cardiobacterium, and Eikenella species.
Haemophilus spp. are present in almost all individuals in lessthan 5% of the microbial population. Fifty percent of them are noncapsulated. H.parainfluenzae makes 10% of the bacterial flora in saliva. Members of the Enterobacteriaceae and non-fermentative Gram-negative bacilli are also present in the oro-pharynx in small numbers or transiently.
Gram-positive bacteria are also predominant microbes that constitute normal flora of the oropharynx. Actinomyces are present in large numbers, comprising 20% of bacterial flora in saliva and on the tongue, 35% in the gingival crev-ices, and 40% in the dental plaque. The ability of Actinomycesspp. to colonize various surfaces is mediated by the fimbriae and other extracellular polysaccharides present in the bac-teria. Other Gram-positive bacilli present in the oropharynx are Actinobacillus, Corynebacterium, Eubacterium, Lactobacillus, Propionibacterium, and Rothia species.
The predominant anaerobes that are found in the oropharynx are Fusobacterium, Bacteriodes, Porphyromonas, Prevotella, and Selenomonas species.Fusobacterium nucleatum is the most common Fusobacterium found in the mouth.
Fungal colonization of the oropharynx is restricted to yeasts only; Candida albicans is present in almost all individuals.
Entamoeba gingivalis and Trichomonas tenax are the only protozoapresent in the oropharynx.
◗ Trachea, larynx, bronchi, and lungs
Colonization of the lower airways is transient with few organisms present at any one time. Long-term colonization may occur when the ciliated epithelial cells are damaged or altered in a disease process.
Gastrointestinal Tract
The gastrointestinal tract can be divided into various distinct anatomical areas. These include esophagus, stomach, jejunum and upper ileum, distal small intestine, and large intestine. The microbial flora present on the mucosa, within crypts, and in the lumen is different. Complete information has been obtained for the stomach and large intestine by studying the microbial composition of feces or the specimens collected during the intra-abdominal surgery.
◗ Esophagus
Sufficient information is not available about the microbial flora of the esophagus. However, transient colonization by oropharyngeal bacteria and yeasts is known to occur.
◗ Stomach
Stomach is an inhospitable organ containing hydrochloric acid and pepsinogen. For this reason, the normal microbial flora is very sparse. The organisms present in the stomach are acid-tolerant Lactobacillus spp., Streptococcus spp., and Helicobacterpylori. H. pylori causes gastritis and gastric and duodenal ulcersand is associated with gastric malignancy.
◗ Jejunum and upper ileum
The number of microbes in the upper part of the small intestine is less than 105/mL of fluid. They are predominantly anaero-bic, consisting ofLactobacillus, Peptostreptococcus, Streptococcus, Porphyromonas, and Prevotella. If upper tract obstruction andstasis occur, then the microbial flora shifts to resemble colonic bacteria, thereby leading to malabsorption syndrome.
◗ Distal small intestine
This is the transition area between the stomach (where a sparse number of acid-tolerant bacteria are found) and the large intes-tine (which is inhabited by a plethora of microbes). The micro-bial population is large (108–109 organisms/g of feces) and diverse with the predominance of anaerobes.
◗ Large intestine
This is the most densely populated organ in the human body. It consists of more than 108 aerobic bacteria and 1011 anaerobic bacteria per gram of feces. Various yeasts and nonpathogenic parasites reside in this area. The bacteria in the large intestine that are present in large numbers includeBifidobacterium spp.,Bacteroides fragilis, Eubacterium spp., Enterococcus spp., and E. coli. Although B. fragilis is the most virulent species,Bacteroidesthetaiotaomicron is more numerous in the colon. Eubacterium spp.is the second most common bacterium in the large intestine. The most commonly isolated species are Eubacterium aerofaciens, Eubacterium cylindroides, Eubacterium lentum, and Eubacterium rectale. Nine species ofBifidobacterium have been isolated infeces. Among Enterococcus species, the most frequently isolated ones are Enterococcus faecalis andEnterococcus faecium.
E. coli causes colonization soon after an infant is born. It isthe most common facultative organism responsible for intra-abdominal infections. Other members of Enterobacteriaceae like Citrobacter spp., Klebsiella spp., Enterobacter spp., and Proteus spp.can establish residence in the intestine.
Streptococcus species and Actinomyces have been isolated fromfecal specimens. A variety of Peptostreptococcus and Gemella species are members of the normal intestinal flora. The spore-forming Bacillus species and Clostridium species are isolated from fecal specimens. Vibrio parahaemolyticuscan also colo-nize the intestinal tract, but only in small numbers. Other organisms commonly isolated in small numbers include species ofFusobacterium, Porphyromonas, and Prevotella species. Various species of Candida and protozoa colonize the large intestine.
Genitourinary Tract
With the exception of female urethra and vagina, the genito-urinary tract is generally sterile. The ureters, kidneys, prostrate, and cervix are normally sterile. The female urethra is colonized with large number of lactobacilli, streptococcal species, and coagulase-negative staphylococci. Fecal organisms, such as E. coli, Enterococcus spp., and Candida spp. can also colonize thefemale urethra, which is transient.
The microbial flora in the vagina is more numerous and diverse. Lactobacilli are the predominant organisms with most commonly isolated species being Lactobacillus acidophilus, Lactobacillus fermentum, Lactobacillus casei, and Lactobacillus cellobiosus. Other anaerobes commonly isolated from thevagina are Bifidobacterium, Peptostreptococcus, Porphyromonas, and Prevotella species.
Actinomyces species are believed to be present in the vaginabecause they are associated with vaginal infections. Actinomycesisraeli is the most common Actinomyces species associated with gen-ital actinomycotic infections. Propionibacterium and Mobiluncus spp. are also present in the vagina.
The aerobic bacteria present in the vagina include coagulase-negative Staphylococcus, Streptococcus (viridans group and beta-hemolytic strains),Corynebacterium spp., Gardnerella vaginalis, Neisseria spp., Haemophilus spp., and members of Enterobacteriaceae.Three species of nonpathogenicTreponema (Treponema phagede-nis, Treponema refringens, and Treponema minutum) are found invaginal specimens. Six species of Mycoplasma andUreaplasma are common inhabitants of vagina, which have pathogenic potential. The flagellate Trichomonas vaginalis is present in small numbers in healthy women. Candida species and Torulopsisglabrata are common members of the microbial flora of vagina.
Body Surface
Human skin is constantly bombarded by organisms present in the environment. The skin is exposed to extremes of tem-perature, moisture, and to chemical disinfectants. There the microbial population is less numerous and complex than at other body sites. The skin is not a homogenous surface. There are relatively dry areas like palms and soles; areas with more apocrine glands, such as axillary, inguinal, and perianal areas; and areas rich with sebaceous glands like forehead and nasola-bial folds. Most organisms proliferate in the moist area. Thus higher densities of microbes are present in areas rich with sweat glands. The skin of face, perirectal area, or groin has a more complex microbial flora than that at other sites (Fig. 75-1).
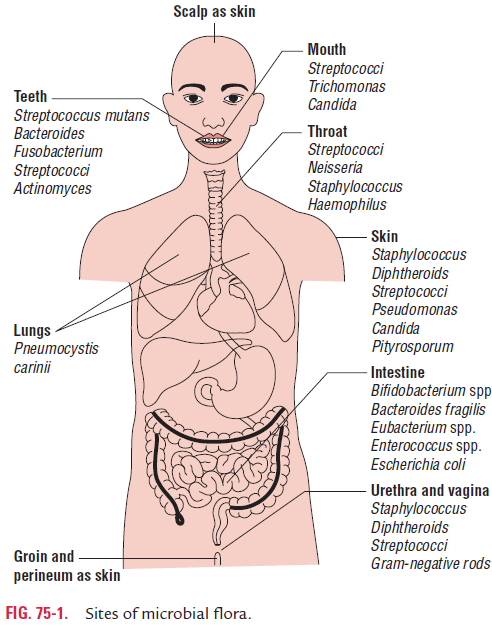
Anaerobic bacteria are 10- to 100-fold more numerous on the skin surface as compared to aerobic bacteria. Gram-positive bacteria predominate over Gram-negative bacteria. The bacteria more commonly recovered from skin surfaces are Staphylococcus spp., Micrococcus spp., Corynebacteriumspp.,
Peptostreptococcus, and Propionibacterium spp. Staphylococcus epidermidis is the most commonly isolated bacterium. Othercoagulase-negative staphylococci found on the skin include Staphylococcus hominis, Staphylococcus haemolyticus, Staphylococcus warneri, and Staphylococcus capitis. Micrococcus luteus is the mostcommon Micrococcus spp. present on the skin and repre-sents 20% of the bacterial population on the head, legs, and arms.Aerococcus viridans, Streptococcus pyogenes, and anaero-bic Peptostreptococcus spp. also establish residence on the skin surface. Corynebacterium species present on the skin surface include Corynebacterium xerosis, Corynebacterium jeikeium, and Corynebacterium minutissimum. The anaerobic Gram-positivebacilli present on the skin surface are Propionibacterium spp. And Clostridium perfringens.
Gram-negative bacteria are generally not recovered from the surface of skin, except during transient colonization.
Acinetobacter spp. organisms have adapted to survive in moistareas of the skin.
Fungal colonization of the skin surface is transient. This includes colonization with yeasts (C. albicans, Malassezia furfur, and Rhodotorula) and dermatophytes. Among these, M. furfur is present in most of the individuals.
Conjunctiva
The flushing action of tears and presence of lysozymes in the tears usually make the conjunctiva free of bacteria. The organ-isms that may be present in the conjunctiva are C. xerosis, Moraxella spp., S. aureus, and nonhemolytic streptococci.
Sterile Sites
The body fluids which include blood, cerebrospinal fluid, syno-vial, pleural, pericardial, peritoneal, and other exudates are nor-mally sterile or transiently infected by microbes.
Some microbes from the mouth and gastrointestinal tract can invade the blood stream in healthy individuals (during tooth brushing or a bowel movement). These organisms are rap-idly removed and are of little significance. Thus, the isolation of an organism from body fluids should be considered significant unless the specimen is contaminated during its collection.
Organ tissues are also generally sterile unless they are infected following systemic spread. Some bacteria like Mycobacterium tuberculosis may be disseminated to lungs, liver,and kidney during initial infection and remain dormant. In this situation, the organism can be recovered from tissue samples. Long-term colonization with organisms like Pneumocystis carinii or latent viruses, such as herpes simplex virus or cytomegalovirus may commonly occur. The external auditory meatus, being an extension of the skin, is colonized primarily by S. epidermidis and diphtheroids.
Human body serves as a home for numerous microbes qual-itatively and quantitatively. They cover the skin and mucosal surfaces; occasionally, they invade into sterile sites to produce disease. These microorganisms act as a barrier to more viru-lent microorganisms, provide vitamins and required growth factors, or exist as commensal inhabitants. The complexity of the microbiota is influenced over time by environmental, host, and microbial factors. Thus, the knowledge of the human microbiota forms a fundamental building block of the normal physiological processes in the human body.
Related Topics