Chapter: Clinical Pharmacology: Anti-infective drugs
Cephalosporins
Cephalosporins
Many antibacterial drugs introduced for clinical
use in recent years have been cephalosporins.
Through the generations
Cephalosporins are grouped into generations
according to their effectiveness against different organisms, their
characteristics, and their development.
§ First-generation cephalosporins include
cefadroxil, cefazolin sodium, and cephalexin monohydrate.
§ Second-generation cephalosporins include
cefaclor, cefprozil, cefoxitin, cefuroxime axetil, and cefuroxime sodium.
§ Third-generation cephalosporins include
cefdinir, cefixime, ce-fotaxime sodium, cefpodoxime proxetil, ceftazidime,
ceftibuten, and ceftriaxone sodium.
§ Fourth-generation cephalosporins include
cefepime hydrochlo-ride.
A sensitive issue
Because penicillins and cephalosporins are
chemically similar (they have what’s called a beta-lactam molecular structure), cross-sensitivity occurs in 10%
to 15% of patients. This means that someone who has had a reaction to
penicillin is also at risk for a reaction to cephalosporins.
Pharmacokinetics
Many cephalosporins are administered
parenterally because they aren’t absorbed from the GI tract. Some cephalosporins
are ab-sorbed from the GI tract and can be administered orally, but food
usually decreases the absorption rate of these oral cephalospo-rins, though not
the amount absorbed. Two cephalosporins (oral cefuroxime and cefpodoxime)
actually have increased absorption when given with food.
Distribution
After absorption, cephalosporins are distributed
widely and readi-ly cross the placenta.
Generational divide
Cefuroxime (second-generation) and the
third-generation drugs cefotaxime, ceftriaxone, and ceftazidime cross the
blood-brain barrier after I.V. or I.M. administration. Cefepime
(fourth-genera-tion) also crosses the blood-brain barrier, but to what extent
isn’t known.
Metabolism
Many cephalosporins aren’t metabolized at all.
Cefotaxime sodium is metabolized to the nonacetyl forms, which provide less
antibac-terial activity than the parent compounds. To a small extent,
cef-triaxone is metabolized in the intestines to inactive metabolites, which
are excreted via the biliary system.
Excretion
All cephalosporins are excreted primarily unchanged
by the kid-neys with the exception of ceftriaxone, which is excreted in stool
via bile.
Pharmacodynamics
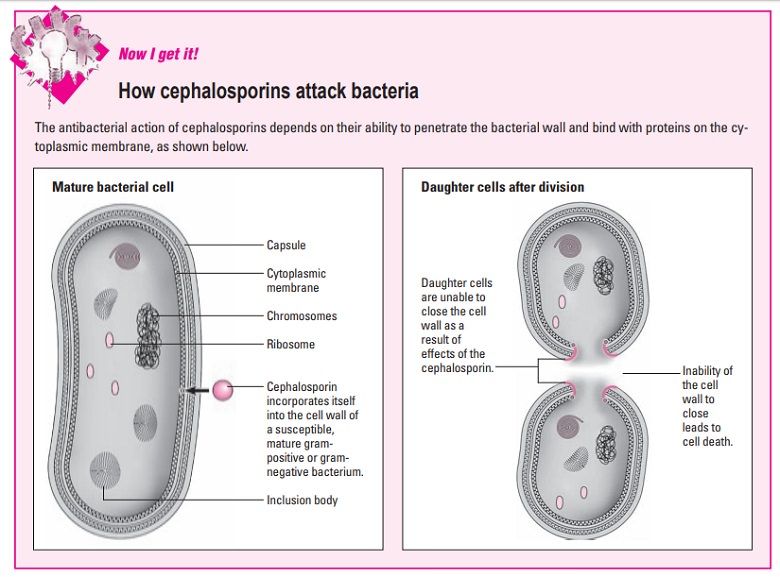
Like penicillins, cephalosporins inhibit cell-wall
synthesis by bind-ing to the bacterial enzymes known as PBPs, located on the
cell membrane. After the drug damages the cell wall by binding with the PBPs,
the body’s natural defense mechanisms destroy the bac-teria. (See How cephalosporins attack bacteria.)
Pharmacotherapeutics
The four generations of cephalosporins have
particular therapeu-tic uses.
§ First-generation cephalosporins, which act
primarily against gram-positive organisms, may be used as alternative therapy
in the patient who’s
allergic to penicillin, depending on how sensitive to penicillin he is. They’re
also used to treat staphylococcal and streptococcal infections, including
pneumonia, cellulitis (skin in-fection), and osteomyelitis (bone infection).
§ Second-generation cephalosporins act against
gram-negative bacteria. Cefoxitin is the only cephalosporin effective against
anaerobes (organisms that live without oxygen).
§ Third-generation cephalosporins, which act
primarily against gram-negative organisms, are the drugs of choice for
infections caused by Enterobacter, P.
aeruginosa, and anaerobic organisms.
§ Fourth-generation cephalosporins are active
against many gram-positive and gram-negative bacteria.
Drug interactions
The patient receiving cephalosporins who drinks
alcoholic bever-ages with or up to 72 hours after taking a dose may experience
acute alcohol intolerance, with such signs and symptoms as headache, flushing,
dizziness, nausea, vomiting, or abdominal cramps within 30 minutes of alcohol
ingestion. This reaction can occur up to 3 days after discontinuing the
antibiotic. (See Adverse reactions to
cephalosporins.)
In use with uricosurics
Uricosurics (drugs to relieve gout), such as
probenecid and sulfinpyrazone, can reduce kidney excretion of some
cephalosporins. Probenecid is used therapeutical-ly to increase and prolong
plasma cephalosporin con-centrations.
Cephalosporins may also decrease estrogen
absorp-tion, leading to decreased efficacy of oral contracep-tives containing
estrogen and progesterone.
Related Topics