Chapter: Pathology: Immunopathology
Autoimmune Diseases
AUTOIMMUNE DISEASES
Systemic
lupus erythematosus (SLE) is a chronic systemic
autoimmune diseasecharacterized by loss of self-tolerance and production of
autoantibodies. Females are affected much more often than males (M:F = 1:9);
peak incidence is age 20–45; and African Americans are affected more often than
Caucasians. The mechanism of injury in lupus is a mix of type II and III
hypersensitivity reactions.
·
Important autoantibodies that may be detected in the sera from lupus patients
include antinuclear antibody (ANA) (>95%); anti-dsDNA (40–60%); anti-Sm
(20–30%); antihistone antibodies; nonhistone nuclear RNA proteins; and blood cells.
·
SLE affects many organ systems
o
Hematologic (type II
hypersensitivity reaction) manifestations can include hemolytic anemia,
thrombocytopenia, neutropenia, and lymphopenia.
o
Skeletal manifestations include an
arthritis characterized by polyarthralgia and synovitis without joint deformity
(type III hypersensitivity reaction).
o
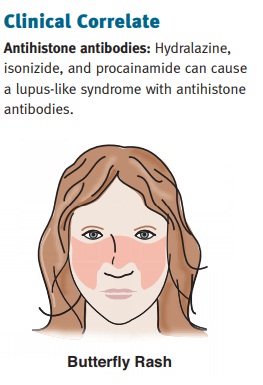
Skin (type III hypersensitivity
reaction) manifestations can include a malar “butterfly” rash; maculopapular
rash; and ulcerations and bullae formation.
o
Serosal surfaces may also be
affected, with resulting pericarditis, pleuri-tis, or pleural effusions (type
III hypersensitivity reaction).
o
Central nervous system
manifestations include focal neurologic symp-toms, seizures, and psychosis
(type III hypersensitivity reaction).
o
Cardiac manifestations include
Libman-Sacks endocarditis (nonbacte-rial verrucous endocarditis) (type III
hypersensitivity reaction).
·
Of particular importance are the renal
manifestations (type III hypersensitiv-ity) classified by the Society of
Nephrology/Renal Pathology Society as follows.
Class I: minimal mesangial lupus nephritis
Class II: mesangial proliferative lupus
nephritis
Class III: focal (< 50%) lupus nephritis
Class IV: diffuse (> 50%) lupus nephritis
Class V: membranous lupus nephritis
Class VI: advanced sclerosing lupus
nephritis
·
Lupus is treated with steroids and immunosuppressive agents. It tends to have a chronic, unpredictable
course with remissions and relapses. The 10-year survival is 85%, with death
frequently being due to renal failure or infections.
Sjögren
syndrome (sicca syndrome) is an autoimmune disease characterized
bydestruction of the lacrimal and salivary glands, resulting in the inability
to produce saliva and tears. Females are affected more often than males, with
typical age 30–50.
Clinical
manifestations include keratoconjunctivitis sicca (dry eyes) and corneal
ulcers; xerostomia (dry mouth); and Mikulicz syndrome (enlargement of the
sali-vary and lacrimal glands). Sjögren syndrome is often associated with
rheumatoid arthritis and other autoimmune diseases. The characteristic
autoantibodies are the anti-ribonucleoprotein antibodies SS-A (Ro) and SS-B
(La). There is an increased risk of developing non-Hodgkin lymphoma.
Scleroderma
(progressive systemic sclerosis) is an autoimmune disease
character-ized by fibroblast stimulation and deposition of collagen in the skin
and internal organs. It affects females more than males, with typical age range
of 20 to 55 years. The pathogenesis involves activation of fibroblasts by
cytokines interleukin 1 (IL-1), platelet-derived growth factor (PDGF), and/or
fibroblast growth factor (FGF) with the resulting activated fibroblasts causing
fibrosis.
·
Diffuse
scleroderma has anti-DNA topoisomerase I antibodies (Scl-70)
(70%),widespread skin involvement, and early involvement of the visceral
organs. Organs that can be affected include the esophagus (dysphagia), GI tract
(mal-absorption), lungs (pulmonary fibrosis which causes dyspnea on exertion),
heart (cardiac fibrosis which may manifest as arrhythmias), and kidney
(fibrosis that may manifest as renal insufficiency).
·
Localized
scleroderma (CREST syndrome) has anti-centromere antibodies,skin
involvement of the face and hands, late involvement of visceral organs, and a
relatively benign clinical course.
Mixed
connective tissue disease is an overlap condition with
features of systemiclupus erythematosus, systemic sclerosis, and polymyositis.
Antiribonucleoprotein antibodies are nearly always positive.
Related Topics