Chapter: Essentials of Psychiatry: Mood Disorders: Bipolar (Manic–Depressive) Disorders
Bipolar (Manic–Depressive) Disorders: Assessment and Differential Diagnosis
Assessment and Differential Diagnosis
Mood episodes are discrete periods of altered feeling, thought and
behavior. Typically they have a distinct onset and offset, be-ginning over days
or weeks and eventually ending gradually after several weeks or months.
Manic–depressive disorder is defined by the occurrence of depressive plus
manic, hypomanic, or mixed episodes, or the occurrence of only manic or mixed
episodes. The diagnostic decision tree for manic–depressive disorder is given in
Figure 47.1.
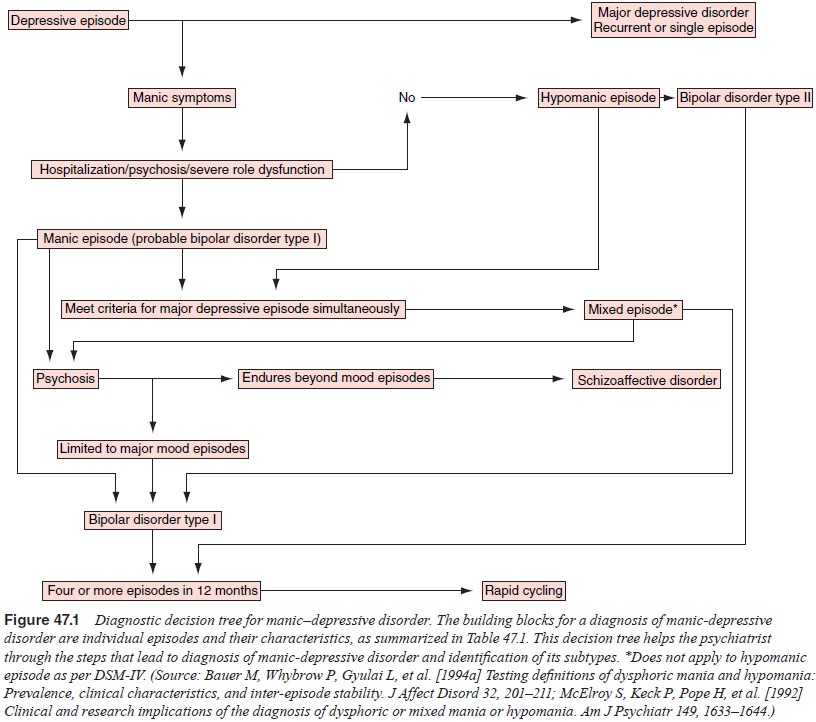
It is important to note that the phenomenologic differentia-tion between
hypomania and mania is not as cut-and-dried. Of the three characteristics by
which one is “promoted” from hypoma-nia to mania, only the presence of
psychosis is firmly grounded in the characteristics of the individual. The
other two character-istics, marked social or occupational role impairment or
hospi-talization, clearly have components that are primarily external to the
individual. If, for instance, one individual has relatively mild manic symptoms
but is living with a family who is unable to tol-erate the behavior, she/he is
more likely to be hospitalized. Simi-larly, the comorbid presence of a severe
disorder is more likely to result in hospitalization and a “promotion” from
type II to type I disorder. Contrarily, limited insurance benefits, or a more
toler-ant family increase the probability that a manic syndrome of a given
severity will be managed without hospitalization and thus be diagnosed as
“hypomania” rather than “mania”.
Related Topics