Chapter: Medical Microbiology: An Introduction to Infectious Diseases: Central Nervous System Infections
Routes of Infection - Central Nervous System Infections
ROUTES OF INFECTION
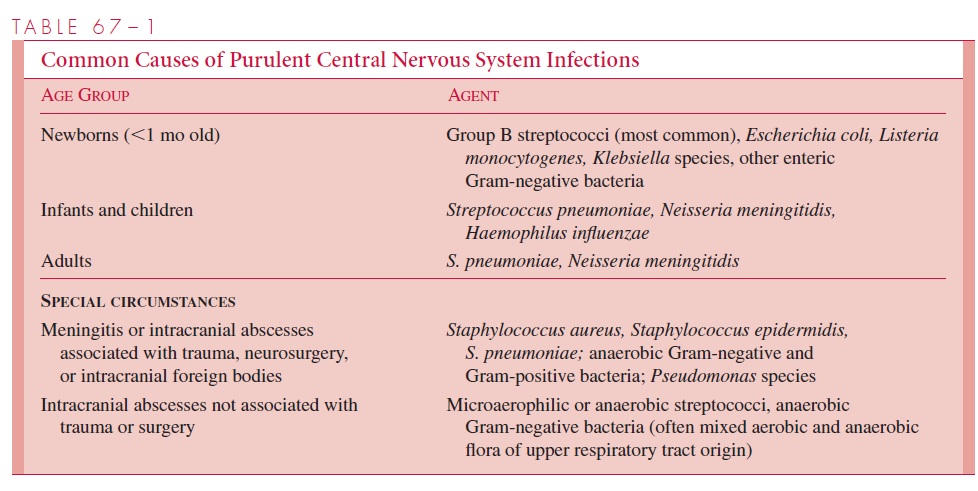
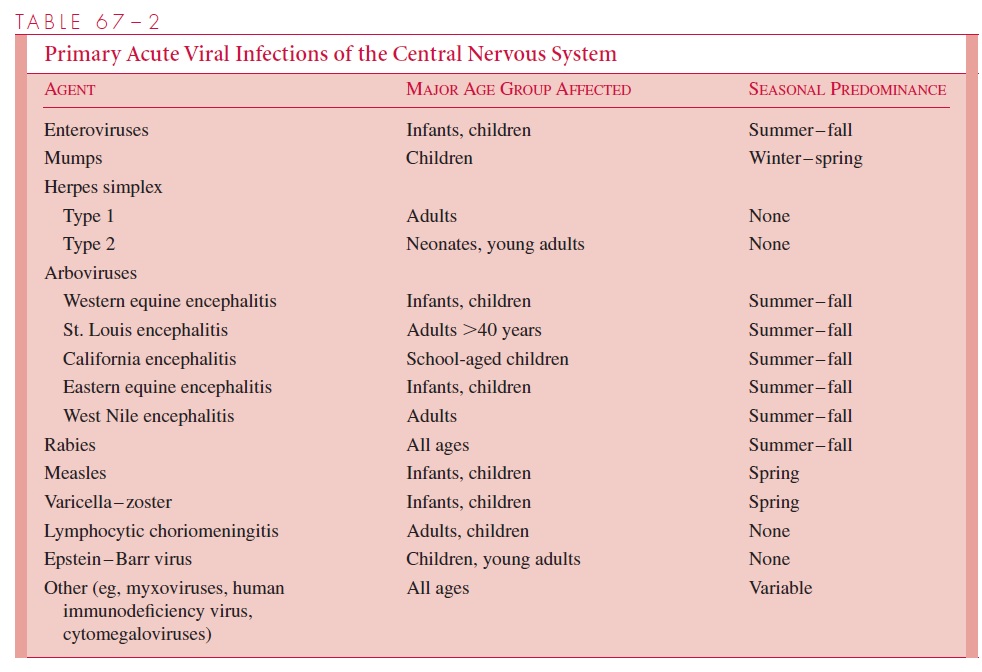
Most CNS infections appear to result from blood-borne spread; for example, bacteremia or viremia resulting from infection of tissue at a site remote from the CNS may result in penetration of the blood–brain barrier. Examples of infectious agents that commonly infect the CNS by this route are Haemophilus influenzae, Neisseria meningitidis, Streptococcus pneumoniae, Mycobacterium tuberculosis, and viruses such as enteroviruses and mumps(Tables 67–1 and 67–2). The initial source of infection leading to bloodstream invasion may be occult (eg, infection of reticuloendothelial tissues) or overt (eg, pneumonia, pharyngitis, skin abscess or cellulitis, or bacterial endocarditis). Occasionally, the route of infection is from a focus close to or contiguous with the CNS. These possible sources in-clude middle ear infection (otitis media), mastoiditis, sinusitis, or pyogenic infections of the skin or bone. Infection may extend directly into the CNS, indirectly via venous path-ways, or in the sheaths of cranial and spinal nerves.
In some cases, a contiguous or distant infectious focus may not be necessary to pro-duce CNS infection. If an anatomic defect exists in the structures encasing the CNS, in-fectious agents may readily gain access to the vulnerable site and establish themselves. Such defects may be traumatically or surgically induced or result from congenital malfor-mations. For example, fractures of the base of the skull may produce an opening between the CNS and the sinuses, nasal passages (defects in the cribriform plate), mastoid, or mid-dle ear. All of these sites are contiguous with the upper respiratory tract, which enables a potentially pathogenic member of the respiratory flora to gain ready access to the CNS. Neurosurgical procedures also create transient communications between the external en-vironment and the CNS that can be readily contaminated. This risk can be compounded when foreign bodies, such as shunts or external drainage tubes, must be left in place for the treatment of hydrocephalus. These foreign bodies, when colonized, can serve as chronic foci of infection. Congenital defects, such as meningomyeloceles or sinus tracts through the cranium or spine, may also be sources. The latter may be overlooked; the ori-fice of the sinus may be a small cleft on the skin surface, or occasionally it may open in-ternally into the intestinal tract. Recurrent purulent meningitis or unusual pathogens in an otherwise healthy host should prompt a careful search for such defects.
Perhaps the least common route of CNS infection is by intraneural pathways. Agents capable of intraneural spread to the CNS include rabies virus (presumably along periph-eral sensory nerves), herpes simplex virus (often, but not exclusively, via the trigeminal nerve root or sacral nerves), polioviruses, and perhaps some togaviruses.
Abscesses of the CNS deserve special mention. Although relatively uncommon com-pared with other CNS infections, they represent a special microbiologic and clinical prob-lem. Such abscesses may be within the tissues of the CNS (eg, brain abscess; Fig 67–1) or localized in the subdural or epidural spaces. They sometimes develop as a complication
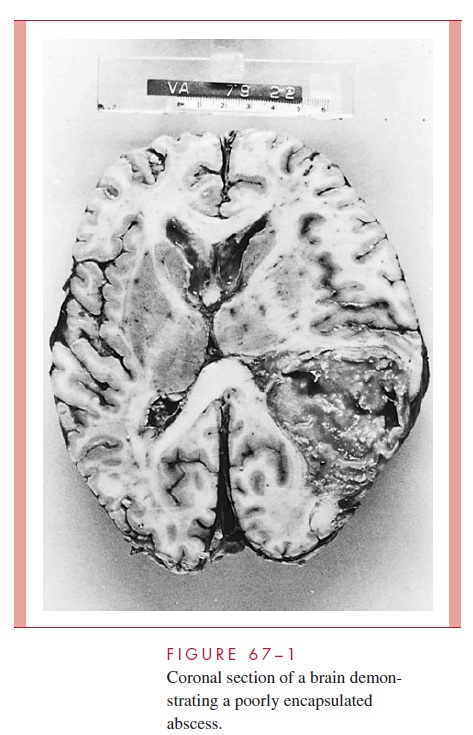
More commonly, abscesses of the CNS result from embolization of bacteria or fungi from a distant focus, such as endocarditis or pyogenic lung abscess; extension from a contiguous focus of infection (eg, sinusitis or mastoiditis); or a compli-cation of surgery or nonsurgical trauma.
Related Topics