Chapter: Medical Microbiology: An Introduction to Infectious Diseases: Herpesviruses
Epstein - Barr Virus : Clinical Aspects
EPSTEIN – B ARR VIRUS : CLINICAL ASPECTS
MANIFESTATIONS
Infectious Mononucleosis
Although most primary EBV infections are asymptomatic, clinically apparent infectious mononucleosis is characterized by fever, malaise, pharyngitis, tender lymphadenitis, and splenomegaly. These symptoms persist for days to weeks; they slowly resolve. Complica- tions such as laryngeal obstruction, meningitis, encephalitis, hemolytic anemia, thrombo- cytopenia, or splenic rupture may occur in 1 to 5% of patients.
Lymphoproliferative Syndrome
Patients with primary or secondary immunodeficiency are susceptible to EBV-induced lymphoproliferative disease. For example, the incidence of these lymphomas is 1 to 2% following renal transplants and 5 to 9% following heart–lung transplants. The risk is greatest in patients experiencing primary EBV infection rather than reactivation. Most characteristic is persistent fever, lymphadenopathy, and hepatosplenopathy.
Burkitt’s Lymphoma
In sub-Saharan Africa, Burkitt’s lymphoma is the most common malignancy in young children, with an incidence of 8 to 10 cases per 100,000 people per year. The risk is great-est in equatorial Africa, where there is a high incidence of malaria. Burkitt’s lymphoma is thought to result from an early EBV infection that produces a large pool of infected B lymphocytes. Malarial infection may further increase the size of this pool and provide a constant antigenic challenge. Serologic screening for increased IgA antibody levels to both VCA and early EBV antigens can be used for early diagnostic purposes.
Nasopharyngeal Carcinoma
Nasopharyngeal carcinoma (NPC) is endemic in southern China, where it is responsible for approximately 25% of the mortality from cancer. The high incidence of NPC among the southern Chinese people suggests that genetic or environmental factors in addition to EBV may also be important in the pathogenesis of the disease.
AIDS Patients
In AIDS patients, several distinct additional EBV-associated diseases may occur, includ-ing hairy leukoplakia of the tongue, interstitial lymphocytic pneumonia (especially in in-fants), and lymphoma.
DIAGNOSIS
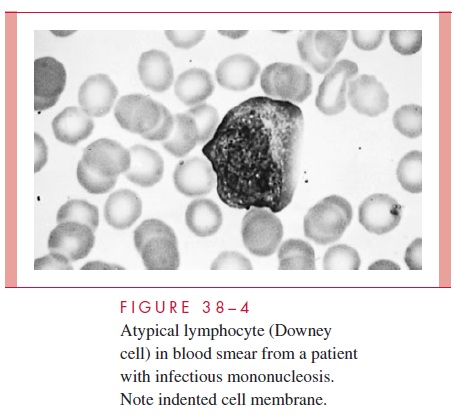
Laboratory analysis of EBV infectious mononucleosis is usually documented by the demonstration of atypical lymphocytes, and heterophile antibodies, or positive EBV-specific serologic findings. Hematologic examination reveals a markedly raised lympho-cyte and monocyte count with more than 10% atypical lymphocytes, called Downey cells (Fig 38– 4). Atypical lymphocytes, although not specific for EBV, are present with the on-set of symptoms and disappear with resolution of disease. Alterations in liver function tests may also occur, and enlargement of the liver and spleen is a frequent finding.
Although not specific for EBV, tests for heterophile antibodies are used most com-monly for diagnosis of infectious mononucleosis. In commercial kits, animal erythrocytes are used in simple slide agglutination methods, which incorporate absorptions to remove cross-reacting antibodies that may develop in other illnesses, such as serum sickness. The infectious mononucleosis heterophile antibody is absorbed by sheep erythrocytes but not by a guinea pig kidney cells. Heterophile antibodies can usually be demonstrated by the end of the first week of illness but may occasionally be delayed until the third or fourth week. They may persist many months.
Approximately 5 to 15% of EBV-induced cases of infectious mononucleosis in adults and a much greater proportion in young children and infants fail to induce detectable lev-els of heterophile antibodies. In these cases, the EBV-specific serologic tests summarized in Table 38–3 may be used to establish the diagnosis. The panel to be tested includes anti-bodies to VCA, which rise quickly and persist for life. Antibodies to EBNAs rise later in
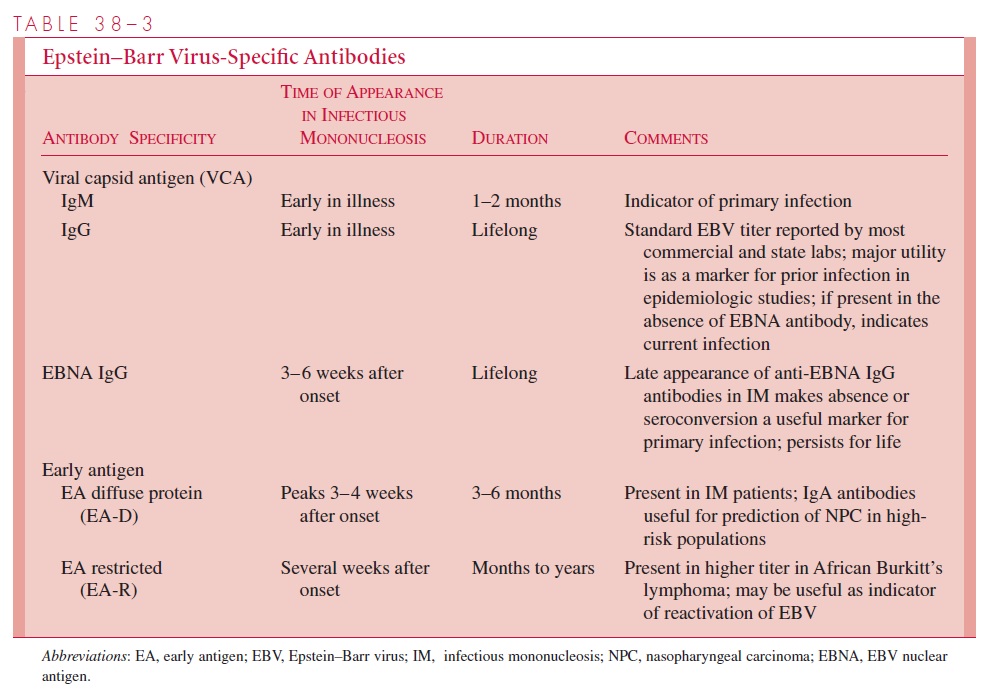
disease (after about 1 month) and also persist in low titers for life. Thus, a high titer to VCA and no titer to EBNA suggests recent EBV infection, whereas antibody titers to both antigens are indicative of past infection. The presence of IgM antibody to VCA is theoretically diagnostic of acute, primary EBV infection, but low levels may occur during reactivation of EBV and cross-reactions with antigens of other herpesviruses occur. Per-sistent antibody to early antigens (anti-EA, -D, or -R) may be correlated with severe dis-ease, nasopharyngeal carcinoma (anti-D), or African Burkitt’s lymphoma (anti-R), but are not useful in diagnosing infectious mononucleosis. Isolation of EBV from clinical speci-mens is not practical, because it requires fresh human B cells or fetal lymphocytes ob-tained from cord blood.
TREATMENT
Treatment of infectious mononucleosis is largely supportive. More than 95% of patients recover uneventfully. In a small percentage of patients, splenic rupture may occur; restric-tion of contact sports or heavy lifting during the acute illness is recommended. The DNA polymerase enzyme of EBV has been shown to be sensitive to acyclovir, and acyclovir can decrease the amount of replication of EBV in tissue culture and in vivo. Despite this antiviral activity, systemic acyclovir makes little or no impact on the clinical illness. Laryngeal obstruction should be treated with corticosteroids. Hairy leukoplakia in AIDS patients does respond to acyclovir treatment.
PREVENTION
The occurrence of Burkitt’s lymphoma and nasopharyngeal carcinoma in restricted geographic areas offers the possibility of prevention by immunization with virus-specific antigen(s). At present, this approach is under exploration. A subunit vaccine has proved effective in preventing the development of tumors in tamarind monkeys, which are highly susceptible to the oncogenic effects of the virus under experimental conditions.
Related Topics